What the experts are saying about another COVID-19 Christmas wave


Keep wearing that mask. Because all we want for Christmas... is Christmas. Photo: Getty
You’d be forgiven for thinking that COVID-19 is just like the rest of us … it really loves Christmas. Well, it loves wrecking Christmas.
It’s bound to happen to some Australian families this year, maybe many.
As you may already have heard, an eighth wave is now in play.
Infections are up, and there’s bound to be a lot more of them.
Some hospitals are already coming under pressure. And an argument has begun as to whether mask mandates should be put in place in the wider community.
It’s more likely that the responsibility for protecting the most vulnerable will be up to the rest of us.
This means:
- Putting on a mask when in crowded venues.
- Maintaining social distancing. Do you remember social distancing?
- Wash your hands often.
- Getting a booster vaccine shot.
- Staying home if we’re unwell.
The reality is removing mandates might have let politicians off the hook. But we haven’t done a great job in protecting our weaker citizens.
On a lighter note: there is some good news to be had.
How many more infections?
There’s appear to no reliable up-to-date figures regarding infections.
News.com.au on Wednesday reported that 6550 cases were reported across the country on October 24, which was when talk of an eighth wave took off.
Professor Adrian Esterman, Chair, Biostatistics and Epidemiology, University of South Australia, told The New Daily:
“Cases are on the rise across the country, although it is becoming more difficult to obtain national data.”
He said only three jurisdictions, South Australia, the ACT, and Tasmania still report weekly data, and even for SA, “they now only report monthly deaths”.
Other jurisdictions, he said, point you to the Commonwealth Department of Health COVID statistics page, which is not particularly helpful.
In the first week of October 2, SA reported around 600 infections. A month later this had blown out to 2500.
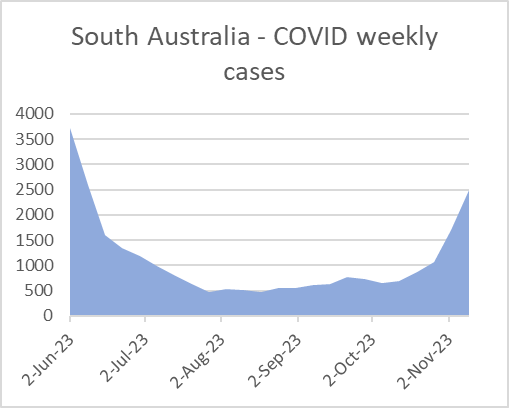
In a month, SA infections steeply grew five-fold.
The most recent health data from NSW shows 4700 infections were reported in the fortnight to November 4. That’s well more than double at the end of September.
At the end of September, the number of cases reported in the previous fortnight was 1800.
The very good news
The seemingly endless parade of sub-variants tend to be more infectious, meaning more people will be getting sick. But the actual illness, in the main, isn’t as vicious or deadly as it was.
Overall, hospitalisations and deaths are both lower than the 2023 winter peak, as well as this time last year.
Professor Esterman said: “As for disease severity, this has not really changed much over the last couple of years.

Professor Adrian Esterman.
“All of these different versions of Omicron mainly infect the upper respiratory passages, tending to cause a milder disease.”
Still, he said, there will be an increase of serious illness.
“Hospitalisations from COVID in SA have been steady for the last four weeks at about 30 patients,” he said.
“But I do expect them to go up as case numbers keep rising.”
What’s causing the new wave?
Professor Esterman said the rise in cases was “probably due to two factors”.
The first: “Waning immunity due to people not keeping up to date with their vaccinations.”
He said, by way of example, “only 23 per cent of Australians aged 65 and over have had an updated vaccination in the last six months.”
Secondly: “Some new highly transmissible variants are taking over in Australia, in particular HK.2 and HV.1. These are descendants of EG.5.1 (Eris) which was dominating.”

Professor Catherine Bennett.
Professor Catherine Bennett is the inaugural chair in Epidemiology at Deakin University. She said one of the new sub-variants could cause COVID to persist through summer.
She said: “There are new sub-variants in the mix now, especially EG 5 and BA 2.86 who were talked about some months back, and that have led to earlier infection surges in overseas countries as they head into their winter.
“EG 5 appears to be driving this wave, but if others take off the we may see a longer wave this summer.”
Mandate masks or leave it up to choice?
Regrettably, there is mixed messaging going on from doctors and health officials.
Two weeks ago, the ABC reported that Victoria’s acting chief health officer had “suggested all Melbournians consider donning masks again as community transmission surges”.
As we reported on Wednesday: in Queensland – where 221 infected people, mostly over the age of 65, are in hospital and two are in intensive care – hospitals and health services have the option to make masks mandatory.
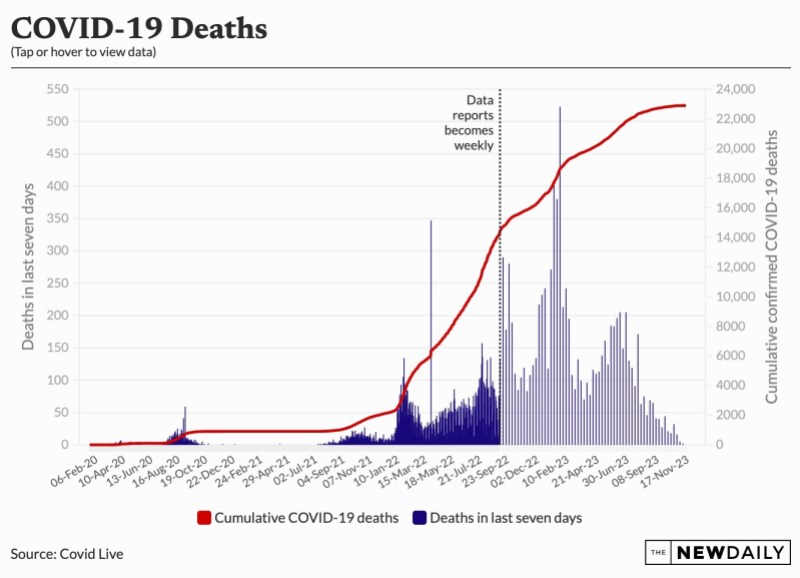
Deaths from COVID-19 are lower than the winter peak, and this time last year.
Australian Medical Association Queensland president Maria Boulton urged people to wear masks in public places such as large crowds, planes and medical settings, to slow the spread of the virus.
She seemed to make a case for masks to be mandated beyond a hospital setting without quite saying so. She noted this would be up to the state’s Chief Health Officer.
“A mask mandate would be the decision of the CHO, but hospitalisations are rising and the health workforce is stretched to breaking point and cannot cope with another overload of patients over the holidays,” she told The Courier Mail.
Queensland CHO Dr John Gerrard responded:
“I am making no general recommendation about mask-wearing in public or in healthcare facilities. That would be disproportionate to the level of risk.”
As far as I can tell, there hasn’t been any uptake of people wearing masks in supermarkets, bars or cinemas. I’ve gone looking.
What do our experts say?
Professor Bennett told The New Daily:
“It’s always sensible to put on masks when background risk is on the rise,” she said.
“I would strongly encourage this in all indoor settings where you can’t keep your distance from others, and when ventilation may be poor and you are there for some time.”

It’s unlikely that masks will be mandated in crowded settings. Photo: Getty
She added it was important to “not go out and mix with others when you have any symptoms, especially those less able to fight off an infection, and for whom an infection could have much more serious consequences”.
Professor Esterman: “We are seeing more hospitals and aged care homes mandating face masks for staff and visitors. Really, this should be a national public health decision and not left to individual institutions.”
Vaccinations number one priority?
Dr Nicole Higgins, President of the Royal Australian College of General Practitioners told The New Daily:
“Perhaps, most importantly, ensure you are vaccinated. If you are 65 and over or have what we call medical co-morbidities, such as a chronic disease, that increases your risk of severe effects, or you are a person with a disability or have complex health needs – it is highly recommended you get a booster dose as well.”
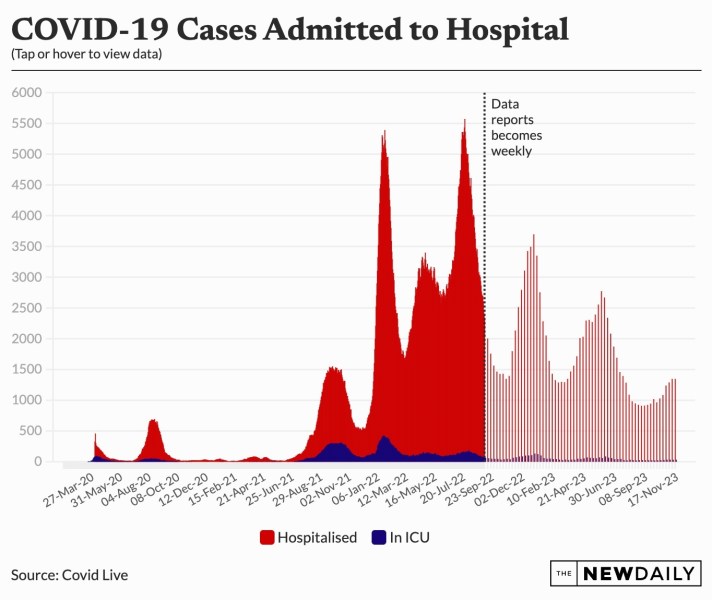
Hospitalisations are lower than the winter peak, and for this time last year.
She added: “If you are an adult aged 18 to 64, you should consider also getting a booster. With high case numbers across Australia, there has never been a better time to book in a vaccination or booster with your GP.”
Dr Higgins suggested that if you know someone in your life who hasn’t been vaccinated or boosted, “why not encourage them to do so. Words from a trusted friend or family member can make all the difference”.
Where are the new vaccines we hear about?
Two new vaccines have been approved by the TGA, one from Moderna and one from Pfizer.
Professor Esterman said these vaccines “are based on the XBB.1.5 strain, and should work extremely well against current circulating subvariants”.
However, it is unclear at the moment when they might be available in Australia.
He said: “Those who are due for another dose and are at high risk, should probably accept the current bivalent vaccine. It is not as effective as the new vaccine but will still give some protection.”
The Therapeutic Goods Administration approved these two COVID-19 vaccines in early October.
They are already available in the United States. EU and UK drug regulators have also approved them.
The Australian Technical Advisory Group says it will assess the vaccines before they’re made available in Australia.
It appears that the big question isn’t when these vaccines will be made available to Australians, but if.
For more, see here.








