AMA criticises hospitals for dragging their feet on anti-COVID measures
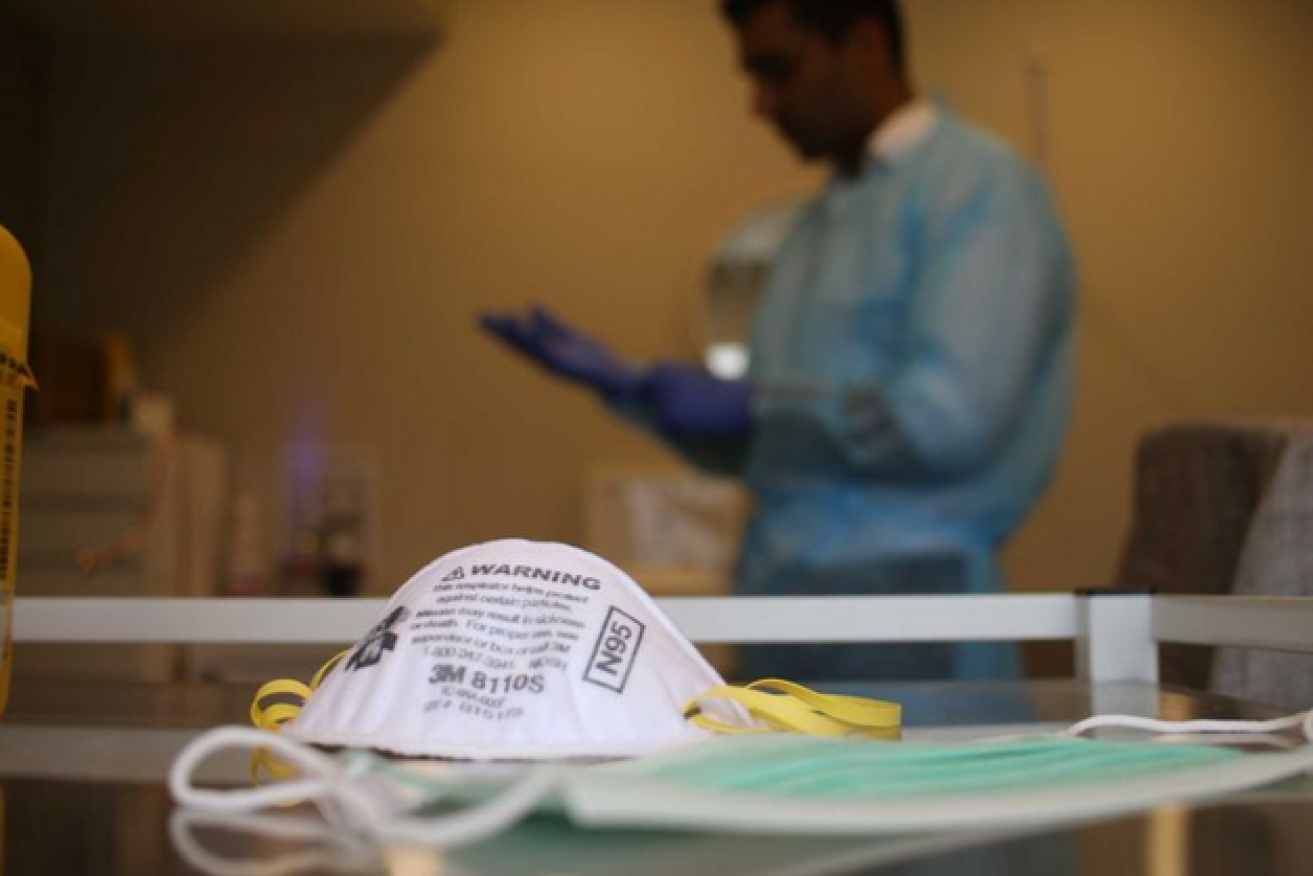
N95 masks offer a higher level of respiratory protection than surgical masks, but are most effective when fit tested. Photo: ABC
The Australian Medical Association (AMA) says some Victorian hospitals have not met the state government’s deadline for a plan to deal with future coronavirus outbreaks, despite the health minister’s assurances.
The Department of Health and Human Services (DHHS) said all healthcare settings were required to have a respiratory protection program in place by October 31, which includes fit-testing staff for N95 face masks, training and risk assessment.
Health Minister Martin Foley said on Saturday that all health settings had met the deadline.
“My understanding is that it has been met,” he said.
“I look forward to receiving a brief in the very near future about how we can continue to drive down those infection rates in our health care workforce, not just for the protection of our healthcare workforce, but for their families their workmates, and of course, their patients.”
There are three healthcare workers who are active cases of COVID-19 in Victoria, and 3,577 healthcare workers have contracted the virus since the start of the pandemic.
A cluster in Melbourne’s northern suburbs that delayed the city’s reopening has been traced back to an infection at the Box Hill Hospital.
Sarah Whitelaw from AMA Victoria said it was good the government required a respiratory plan to prevent the virus spreading at healthcare settings, but the experience of staff was that the plans had not been completed.

Australian Medical Association Victoria board member Sarah Whitelaw says the Government’s statements are at odds with doctor experiences on the ground. Photo: ABC
“It is disconcerting and really stressful for staff to to hear public announcements that are just so far from their experience on the ground, and we have been feeding back that message really strongly,” she said.
Dr Whitelaw said some hospitals had completed a respiratory protection program, including fit-testing for staff who required N95 masks and an audit of ventilation.
She said others would finish in the next couple of months, but several hospitals had not yet even bought the machine required to do fit testing.
“Some hospitals haven’t started,” she said.
“This is a really widespread problem, we’re not talking about just one or two.
“We know that there’s staff shortages, we know that there are resource limitations, so it’s not about expecting the impossible, it’s about saying what’s going on here, why haven’t we met the timelines we haven’t been able to meet, and what do you need to make it happen?”
Dr Whitelaw said there needed to be more communication with staff in clinical settings.
“It’s one thing to develop a plan and it’s quite another to be able to ask clinicians and staff on the ground what do you need to make this happen, how long is it going to take, what extra resources do you need to make this happen,” she said.
“Victoria now has some of the best guidelines in the country with regards to respiratory protection programs, but that’s a long way from the reality of putting those into practice.”
A spokesperson for the DHHS said work had also begun on auditing ventilation in clinical settings, which was promised in August
‘It only takes one patient’
Infectious diseases physician Michelle Ananda-Rajah is calling for a regular audit of respiratory plans in healthcare settings, including fit testing and ventilation.
“It would be absolutely foolhardy to assume that we’re not going to have any more COVID patients hospitalised, and it only takes one patient with COVID to spark an outbreak which seeds back into the community,” Dr Ananda-Rajah said.
“We can’t afford to have that as we move into a recovery.”
She said there was a lot of variation in COVID plans across Melbourne’s hospitals.
“It’s not clear as to why that’s the case, why there’s so much variation in these health services, and I think questions really need to be asked about that,” she said.
Want to see more stories from The New Daily in your Google search results?
- Click here to set The New Daily as a preferred source.
- Tick the box next to "The New Daily". That's it.








