Could antivirals cut long COVID risk? What research says on prevention and treatment

A protester holds up a placard demanding research into Long COVID-19. Photo: Getty
Evidence is continuing to accumulate on the burden and frequency of chronic effects after a COVID-19 infection, which fall under the umbrella term “long COVID”.
At least 5 per cent to 10 per cent of people who contract COVID experience long COVID.
This can include symptoms (for example, fatigue, brain fog and breathlessness) or conditions (for example, heart conditions, neurological conditions and diabetes) after the initial infection that may be persisting, new or relapsing.
Studies show the symptoms and increased risk of chronic conditions can persist for up to two years after infection.
The individual impact of long COVID can range from temporary to severely disabling, and the societal cost – for example due to reduced workforce and increased health care costs – is enormous.
The lower risk of developing long COVID with up-to-date COVID vaccinations is substantially offset by the high levels of infections and reinfections globally.
As a result, the cumulative burden of long COVID has increased, including in lower- and middle-income countries. A conservative estimate suggests 65 million people may be currently affected globally.
So where are we at with reducing the risk of, and treating, long COVID?
Could antivirals reduce the risk of long COVID?
COVID antiviral drugs, taken orally, continue to play an important role in reducing acute severe disease after infection. In Australia, they’re available to those at highest risk from COVID.
Observational research has suggested taking antivirals during a COVID infection can reduce the risk of long COVID in people with at least one risk factor for acute severe COVID.
In one study, nirmatrelvir and ritonavir, known as Paxlovid, was associated with a 26 per cent reduced risk of developing long COVID. It was also linked to a 47 per cent reduced risk of death and a 24 per cent reduced risk of hospitalisation after the acute infection phase.
A similar 14 per cent reduction in long COVID risk has been reported for molnupiravir (Lagevrio).
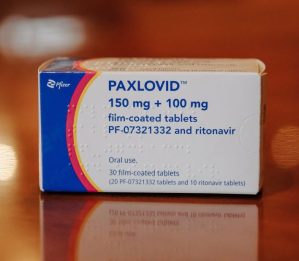
Some research suggests taking Paxlovid during a COVID infection could reduce the risk of long COVID. Photo: Getty
Ensitrelvir – a COVID antiviral available in Japan – could also reduce the risk of long COVID, preliminary analyses suggest.
More research is needed, but this data indicates antiviral medications may be a key approach to lessening the risk of long COVID.
The population most at risk of long COVID (often working-age adults) differs from those most at risk of severe disease from a COVID infection (older adults or those with chronic medical conditions).
Eligibility criteria to access antivirals do not currently include consideration of long COVID.
Meanwhile, one randomised trial found metformin, a commonly prescribed diabetes medication, could also reduce long COVID risk.
The study offered people with symptomatic COVID who were overweight or obese metformin for two weeks (beginning within a week of symptoms starting). This group was 41 per cent less likely to develop long COVID compared with a placebo group that didn’t take metformin.
The way this works might involve an effect on the powerhouses of our cells, mitochondria, or directly on the virus. Whatever the precise mechanism, further research should be prioritised to fast-track this potential.

COVID is still a threat, so long COVID is too. Photo: Getty
We’re understanding more about long COVID
There are no effective or approved treatments for long COVID at present.
Currently about 12 clinical trials are testing potential drugs. A number of candidate treatments exist for certain components of long COVID that may be useful in subgroups of patients.
However, recently we’ve seen major advances in understanding what’s actually driving long COVID in the body. This knowledge opens up approaches for both diagnosis and treatments or interventions.
Research on treatments is lacking
An Australian parliamentary inquiry into long COVID stressed the best way to avoid the condition is to lower the risk of getting infected with COVID in the first place (through protective behaviours such as vaccination, mask wearing and cleaner indoor air).
While these are all important measures, we would benefit from having more tools at our disposal to prevent and treat long COVID. After all, COVID is still evolving rapidly and vast numbers of people are likely to be reinfected in the months and years ahead.
Overall, the quantity and speed of clinical trials into long COVID treatments has been insufficient. And most public health policy approaches are focused on preventing severe disease from a COVID infection, rather than the long-term effects.
That said, Australia recently announced an initial $22 million of funding and a plan for research into long COVID through the Medical Research Future Fund.
In July 2023, the White House established the Office of Long COVID Research and Practice which will co-ordinate the US government’s response to long COVID, as well as two randomised trials of Paxlovid.
What now?
Given what we now know about long COVID, and the additional concern of what we don’t know (for example, could organ damage reveal itself many years down the track?), we desperately need diagnostic tools, clinical care pathways coupled with health worker training, and treatments to prevent and cure long COVID.
Unaddressed, long COVID may well lead to a new and substantial health and societal burden for many years to come.
The response must involve prioritisation of research, such as that which led to the fast development of COVID vaccines and antivirals.
There are some positive signs in the policy and research space, but we need to see stronger recognition of long COVID and a greater sense of urgency around finding solutions.![]()
Suman Majumdar, Associate Professor and Chief Health Officer – COVID and Health Emergencies, Burnet Institute; Brendan Crabb, Director and CEO, Burnet Institute; Emma Pakula, Senior Research and Policy Officer, Burnet Institute; Michelle Scoullar, Senior Research Fellow, Burnet Institute, and Ziyad Al-Aly, Director Clinical Epidemiology Center, VA St. Louis Health Care System, Washington University in St Louis
This article is republished from The Conversation under a Creative Commons licence. Read the original article.